Lung abscess (Lungenabszess)
General information:
- Result of a necrotizing pneumonia (e.g. after aspiration of gastric juice, GER).
- Streptococci, Staphylococcus aureus, Klebsiella pneumoniae, Pseudomonas aeruginose, or other gram – negative enteric organisms have been found to be responsible.
- Frequent in children with neurological impairment, seizure disorders and immune suppression.
- Location: posterior segment of the right upper lobe and the superior segments of the right and left lower lobe.
- 10% of the affected children have more than one abscess.
- Notice the probability of an abscess formation in etiological connection with an unknown pre-existing localized pulmonary malformation (CCAM, bronchogenic cyst, lung cyst, infected sequestration).
Symptoms:
- Cough, fever, tachypnea, decreased (no) breathing sounds and dullness to percussion on the involved side.
- Respiratory distress.
- Pulmonary infiltrate, cavity with fluid level.
- Usually quick development of pleural effusion.
- Perforation into the pleural cavity leads to empyema usually combined with pneumothorax.
Diagnostic workout:
- Thoracic X-ray, CT or MRI scan.
- Bronchial lavage guided by flexible fiberoptic bronchoscopy or thoracocentesis is useful in obtaining culture material used to determine specific antibiotic treatment.
Indication for operation:
- Bronchopleural fistula.
- Operation frequently needed in younger and more debilitated children.
- Large abscesses (approx. more than 5 cm in diameter) with fluid levels, especially located near the lung surface, unresponsive after aggressive conservative treatment.
- No complete expansion of the lung over a period of about two weeks.
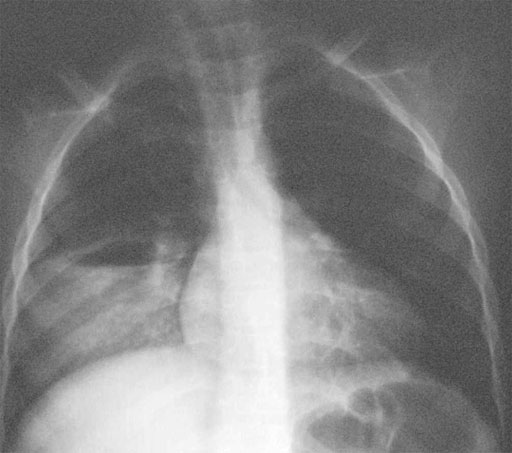
Right lung abscess
Treatment/Operation:
- Intravenous antibiotic management continued orally.
- Closed drainage (multiple chest tubes sometimes necessary).
- Open drainage (including decortication) of the pleural effusion usually with two large chest tubes.
- Resection, usually of the complete involved lobe (covering the bronchial closure additionally with a dorsally based intercostal muscle flap). Care must be taken with the induction of anaesthesia or positioning the patient to prevent a spill of the abscess contents into the contralateral lung (bronchoscopically guided suction before!).
Postoperative management:
- Chest tubes may be removed if the lung is fully expanded and drainage volumes decrease below 20 to 50cc during a 24 hours period.
- Antibiotic management continued orally after release from the hospital.
Prognosis:
- Good.
- Resolution of a sufficiently drained abscess needs several weeks.
Pneumatocele
General information:
- Thin walled, air filled cyst usually after a necrotizing Staphylococcus aureus pneumonia (other germs involved: Streptococcus, Hemophilus influenzae, Klebsiella, E. coli and Pseudomonas).
- Endotoxin released from the staphylococcal organisms contributes to the extremely destructive inflammatory process.
- Mechanically ventilated patients are at increased risk of developing pneumatocele.
- Adjacent structures may be compressed or a mediastinal shift may occur, when tension pneumatocele develops.
- 25% of the pneumatoceles rupture, causing a usually insignificant pneumothorax.
Symptoms:
- Respiratory insufficiency.
Diagnostic workout:
- Thoracic X-ray or CT scan.
- Thoracic ultrasound.
Indication for operation:
- Rapidly enlarging pneumatocele producing mediastinal shift (tension pneumatocele).
Treatment/Operation:
- Most pneumoatoceles require no treatment, just observation.
- Percutaneous needle aspiration or chest tube for drainage in large cysts.
- Thoracotomy, suture or resection is rarely necessary.
Postoperative management:
- Chest tubes may be removed if the lung is fully expanded and drainage volumes decrease below 20 to 50cc during a 24 hour period.
Prognosis:
- Good. About 50% resolve within 6 weeks and the remainder within 12 months.



