Foreign body aspiration
(Fremdkörperaspiration, Aspiration)
General information:
- Patients between the age 1 and 3, most common at age 2 (toddlers).
- Aspirated material: peanuts, popcorn, seeds, pieces of meat, or other small objects.
- Larger objects may lodge within the glottic opening (cause of death, especially in the group around the age of one).
- Smaller objects are usually inhaled into the more distal branches of the airways (frequent location: right or left main bronchus, right and left bronchi of the lower lobes).
- Significant local inflammation usually starts 2 – 3 days after aspiration.
Symptoms:
- Coughing, wheezing, suprasternal retractions.
- Respiratory distress, cyanosis.
- In cases of minor aspiration, unspecific symptoms comparable to those seen in respiratory infections.
- Pneumonitis after prolonged occlusion.
- Atelectasis after complete occlusion.
- Tracheal deviation, mediastinal shift.
Diagnostic workout:
- Anamnesis (extraordinary episode of coughing, peanuts ?).
- Thoracic X-ray with over inflation of the involved lung (air entrapment due to a ball – valve effect), possibly mediastinal shift.
- Flexible fiberoptic or classically the rigid laryngo – bronchoscopy carried out synchronously with the endoscopically guided extraction.
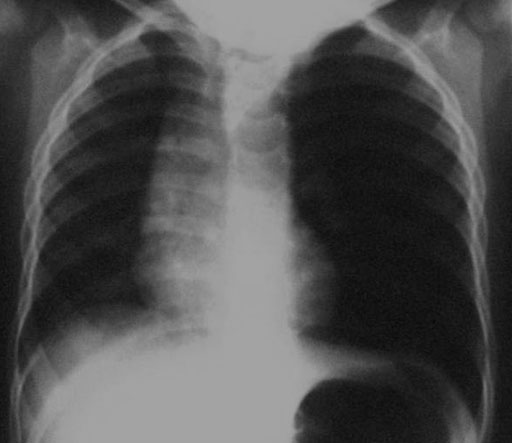
Over inflated left lung due to aspiration
Treatment/Operation:
- Heimlich manoeuvre (designed to force the diaphragm upward, which generates increased intrathoracic pressure) to dislodge a large foreign body from the larynx
- Rigid laryngo – bronchoscopy under general anaesthesia and extraction of the foreign body (effective in 95% with a complication rate of less than 1% using the bronchoscope, telescope with mounted forceps, alligator forceps, peanut forceps, balloon catheter, basket forceps, suction and lavage catheters. Avoid high ventilatory pressures which could drive the foreign body further into the airway).
- Very rarely thoracotomy, bronchotomy or sometimes localised lung resection is necessary.
Postoperative management:
- Plain control X-ray.
- In questionable cases repeated bronchoscopy.
Prognosis:
- Good, directly related to the timeliness of diagnosis and treatment.



