Congenital cystic adenomatoid malformation
(Zystisch adenomatoide Malformation, CCAM):
General information:
- Non-cystic or multi-cystic mass of pulmonary tissue lined by cuboidal or columnar epithelium (sometimes skeletal muscle can be detected in the cyst wall). There is an overgrowth of bronchioles with suppression of the alveolar development.
- Usually only a single lobe is affected.
- The lesion can become larger because of fluid and air trapping. Over-distension of the involved lobe may lead to mediastinal shift, anasarka, hydramnion, hypoplasia of the ipsilateral and contralateral lund, fetal death, or respiratory distress after birth.
- 3 Types:
- Type I (50-75%): Single or multiple cysts more than 2 cm in diameter, lined by ciliated pseudostratified columnar epithelium with thick smooth muscle and elastic tissue walls.
- Type II (10-40%): Multiple small cysts less than 1 cm in diameter, lined by cilitaed cuboidal or columnar epithelium. Respiratory bronchioles and distended alveoli may be present between these cysts. This type is frequently associated with other congenital anomalies (renal agenesis, heart defects).
- Type III (10%): Non-cystic adenomatous solid mass. Poor prognosis.
- Spontaneous regression is possible.
- Risk of pneumothorax, infection and malignant change (small risk).
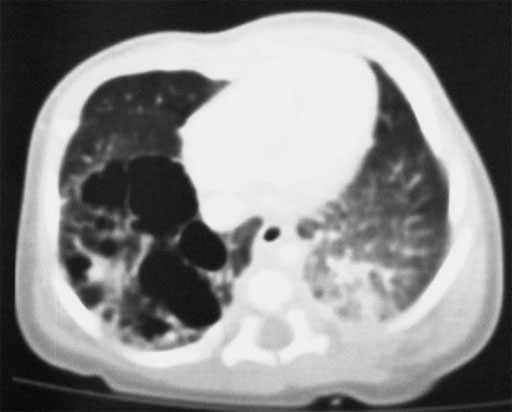
CT scan showing a CCAM in the right lung
Symptoms:
- May be asymptomatic.
- Respiratory distress in Type II and III.
Diagnostic workout:
- Prenatal serial ultrasounds (detectable in the 12th to 14th gestational week).
- Repeated X-ray, CT scan or MRI.
Indication for operation:
- Fetal intervention (before the 32nd week) in severe cases with medistinal shift: Thoracocentesis of large cysts or resection of the lesion in utero.
- Persistent (no signs of regression after 3 months of observation) and growing lesion, even if the patient is asymptomatic.
Treatment/Operation:
- Thoracotomy and usually lobectomy within the first year of life.
Postoperative management:
- Chest tubes may be removed if the lung is fully expanded and drainage volumes decrease below 20 to 50cc during a 24 hour period.
- Problem of pulmonary hypertension and shunting may provoke ECMO (after successful resection) support.
Prognosis:
- Macrocystic lesions (> 5mm): good prognosis.
- Microcystic lesions (< 5mm): poor prognosis.



